Modernize and streamline data exchange
Ensure ongoing compliance and deliver a better member experience with our award-winning interoperability platform.
Design, automate, and administer value-based contracts
The complexities of value-based contracting and payments make it difficult for healthcare organizations to effectively monitor contract performance and ensure accurate payments. Not only does this affect their ability to create reliable financial forecasts, it also makes it harder to expand their value-based operations and move into more complex alternative payment models (APMs).
Edifecs’ cloud-native value-based payment solutions are purpose-built to connect payers and providers, deliver transparency, and establish a single source of truth in value-based programming.
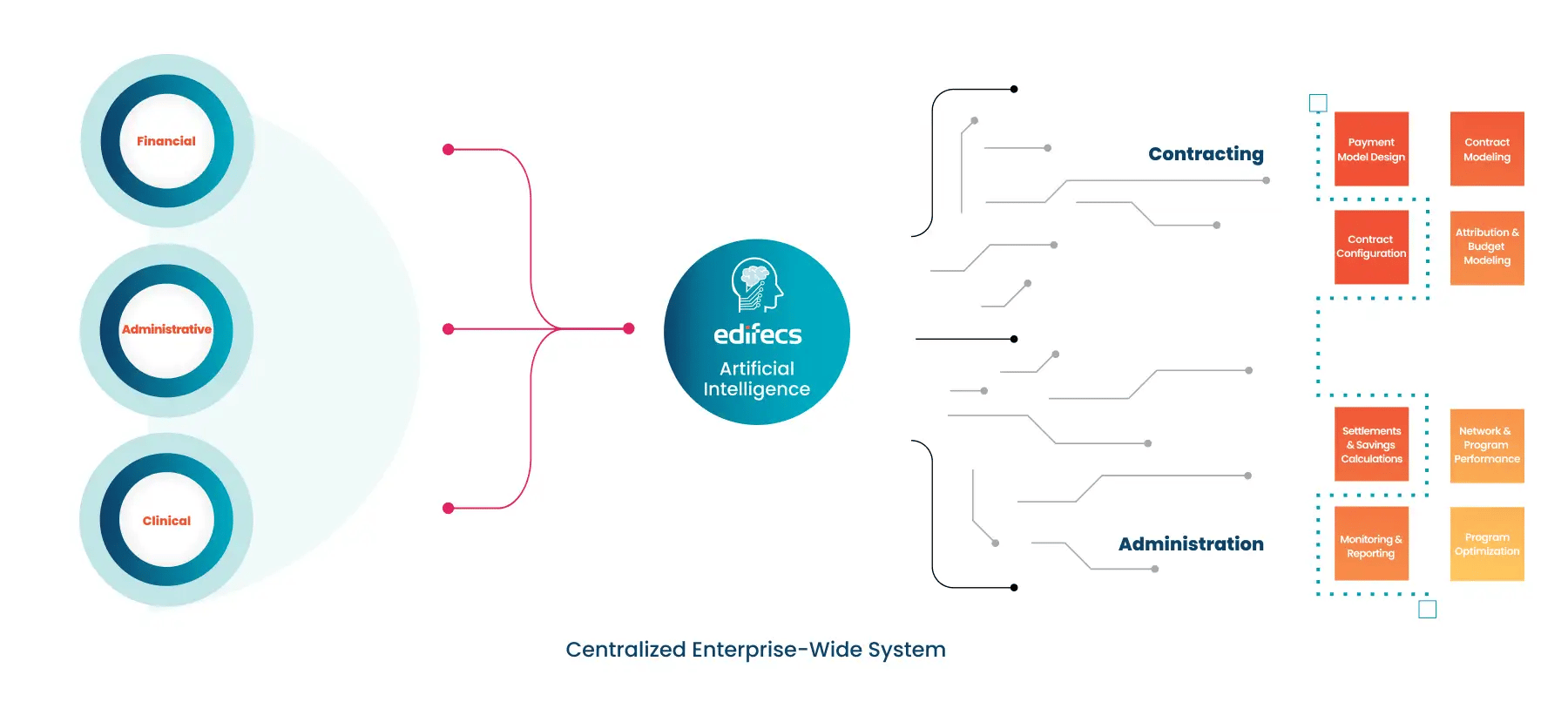
Ensure ongoing compliance and deliver a better member experience with our award-winning interoperability platform.


Population Payment Management
Edifecs' Population Payment Management solution can help healthcare organizations overcome those challenges and accelerate the shift to value.
Why is value-based care a priority for healthcare organizations?
Moving from traditional fee-for-service arrangements to value-based care—which emphasizes early intervention and ongoing patient engagement—offers a variety of benefits for health plans, providers, and patients.
VBC’s focus on preventive care helps reduce the likelihood of hospitalizations or the development of avoidable comorbid conditions, enabling better care outcomes and improving satisfaction and engagement for patients/members. This approach, coupled with more effective and patient-centered care coordination, helps minimize unnecessary expenses and reduces care costs across the healthcare spectrum.
Why hasn’t healthcare fully adopted value-based care?
Although CMS has set a goal of transitioning all Medicare beneficiaries and “the vast majority of Medicaid beneficiaries” to value-based care by 2030, many healthcare organizations have been slow to make the transition for a few key reasons:
What are alternative payment models (APMs)?
Under the traditional fee-for-service (FFS) model, healthcare providers are financially incentivized to maximize visit volume—often at the expense of delivering more comprehensive care.
APMs reward providers based on the quality—not the quantity—of the care they deliver, empowering providers to take a more patient-focused approach that prioritizes preventive care and early intervention and supports better long-term health outcomes.
What are the most common APMs?
Though there are a variety of different APMs, some models have gained more widespread adoption than others. The most common APMs in use in healthcare include: